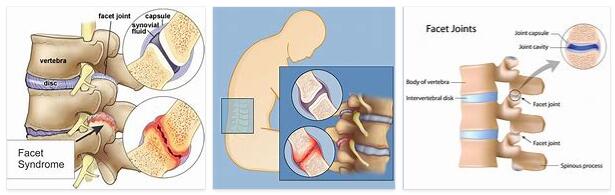
The so-called facet syndrome (often also facet joint syndrome) is a painful disease of the joints that are located between the individual vertebral bodies. The condition is one of the most common causes of back pain and has been linked to herniated discs. The trigger of the syndrome is usually too little distance between the individual vertebral bodies, which is considered a sign of wear and tear.
What is Facet Syndrome?
According to gradphysics.com, facet syndrome is a disease of the joints that are located between the individual vertebral bodies of the human spine. The disease is therefore also known as facet joint syndrome or vertebral joint arthrosis.
The terms are used synonymously. However, all common terminologies are collective terms. This means that symptoms that can be traced back to different causes are grouped under the term facet syndrome. The course of the disease is therefore not always identical.
Causes
Facet syndrome can have a number of causes. In most cases there is a reduction in the distance between the vertebral bodies due to wear and tear. This is what causes the severe pain. Experts speak of degenerative damage to the vertebral joints. Damage to the intervertebral discs should also be considered.
Because this too can lead to the development of a facet syndrome. After all, the facet joints and the intervertebral disc are closely interrelated due to their similar function. It follows that damage to the intervertebral discs often leads to damage to the facet joints and vice versa.
Another cause of facet syndrome can be inflammation of the joints (arthritis). In addition, cysts and ganglia (proliferation of connective tissue) are also potential causes of vertebral joint arthrosis. This is especially true if these form near the vertebral joints.
The literature also reports that spinal stenosis can lead to the development of a facet joint syndrome. Spinal canal stenosis is when the spinal canal narrows. In these cases, nerves or immediate joint damage can also occur.
In addition, tumors and the stress of childbirth can lead to a misalignment of the spine, so that this must also be seen as a cause for the development of a facet syndrome. However, this is rare.
Symptoms, ailments & signs
Facet syndrome manifests itself primarily through noticeable pain. Patients describe it as dull. Often it is not possible to locate the location exactly. But some also speak of piercing pain.
It is characteristic that the pain intensity varies throughout the day. Usually an increase is recorded as the day progresses. This is explained by the stress on the spine that arises from walking upright. Because the spine rests at night, it can also feel stiff in the morning. In addition to back pain, those with facet syndrome usually suffer from hip problems.
Occasionally, leg cramps can also occur. This is because the back pain has a radiating effect. This is especially true when the spine is under heavy strain. Because of the pain, many of those affected have a significant impact on their everyday lives.
Diagnosis
The diagnosis of facet syndrome can be made by the family doctor or an orthopedic surgeon. Usually, the general practitioner’s initial diagnosis is subsequently confirmed by the specialist. A doctor first diagnoses the syndrome using a standardized pain questionnaire.
This determines the type, duration, frequency and intensity of the back pain. If this results in a suspicion, further investigations will follow. First, an X-ray image is usually made from two different directions. This allows, among other things. Tumors can be excluded as the cause.
It is also common to do an ultrasound scan. This avoids exposure to radiation. However, an exact examination of the spinal cord space, as is necessary to establish a definitive diagnosis, can only be carried out using computed tomography (CT) or magnetic resonance imaging (MRT).
Complications
With facet syndrome there is severe back pain in most cases. These occur mainly during physical exertion or during sporting activities and can severely restrict the patient’s everyday life. The pain often cannot be localized directly, but it is felt to be stabbing.
It is not uncommon for patients to suffer from hip discomfort and progressive pain that worsens over time. These complications make everyday life difficult, so that pain-free movement is no longer possible. The severe pain can also trigger depression and other psychological complaints.
Treatment should take place early in order to avoid surgical interventions. Physiotherapy or pain therapy is mainly used. Pain relief medications can also be taken, but these can damage the stomach in the long run.
The therapies are not always successful, but they can severely limit the facet syndrome. Since surgical interventions are in most cases not possible if the joint is damaged, they are only used if there are problems with the nerves. Complications only arise when nerves are pinched or otherwise damaged.
When should you go to the doctor?
Facet syndrome requires medical evaluation and treatment. If left untreated, the syndrome can lead to various restrictions in movement and thus to a significantly reduced quality of life for the patient. People should see a doctor if they experience severe pain in the hip area. The pain itself is boring and in many cases cannot be localized very precisely. The pain often occurs throughout the day and significantly restricts the person’s everyday life.
Stiff joints after getting up can also indicate facet syndrome. Other hip problems are also a symptom of this disease. The pain can radiate to other regions, so that severe pain can also occur in the back. In most cases, the examination and treatment of facet syndrome is carried out by an orthopedic surgeon or through various therapies.
This can limit most complaints. However, since the syndrome can also lead to psychological complaints, psychological treatment should be carried out in parallel. Pain can be limited with the help of pain relievers, but these should not be taken over a long period of time.
Treatment & Therapy
If facet syndrome is diagnosed at an early stage, treatment can be conservative (i.e. without surgery). This form of treatment is mainly carried out through passive movement, as can be achieved through physiotherapy. In addition, physiotherapy and massages are used.
If possible, the back is specifically strengthened through muscle building. This relieves the spine, which reduces pain. Conservative therapy is usually accompanied by drug treatment. The patients receive preparations to relieve pain and to prevent inflammation (for example paracetamol).
In particularly serious cases, opioids are also used. However, this is the exception. Severe cases, on the other hand, are treated surgically. A number of minimally invasive procedures are available for this. The aim is to treat the pain-conducting nerve tracts.
The surgeon regularly injects a pain reliever. Elaborate operations are the exception in the treatment of facet syndrome. However, here, too, only the nerves are targeted, because an improvement in joint damage is usually not possible.
Outlook & forecast
The prognosis for a facet syndrome can vary greatly. It depends, among other things, on the lifestyle of the person affected, on other wear and tear on their spine and on therapeutic measures.
If facet syndrome is dealt with quickly with physical therapy, the chances of relief are good. The built-up muscles can relieve the vertebral joints and prevent further wear and tear. However, this only works if the recommended training is carried out consistently. In addition, the person concerned should avoid actions that put wrong or excessive strain on his or her spine. Nevertheless, it should be noted that accidents or individual actions can still lead to a worsening of suffering.
Other methods of pain treatment usually only temporarily relieve the suffering. In addition, no causal improvement in the condition can be expected without invasive interventions. If, on the other hand, an operative procedure is chosen (facet denervation; joint stiffening), the prognosis is good. Pain may go away in whole or in part, until either the joint prolapses or the nerves have regenerated. If this is the case, the minimally invasive procedure can easily be repeated.
The prognosis is good overall with proper training to relieve stress and a healthy body weight. In addition, most cases of facet syndrome are easily treatable thanks to pain therapies and operations.
Prevention
Facet syndrome is difficult to prevent in a targeted manner. However, a muscular back is a good way of avoiding damage to the spine. Strengthening the back muscles can therefore be regarded as a suitable preventive measure.
Aftercare
As a rule, the follow-up measures for facet syndrome are very limited. Since this is a largely unexplored disease, in which a complete cure is not always possible, these possibilities are greatly reduced. For this reason, facet syndrome focuses on the early detection and treatment of the disease so that there are no further complications and complaints.
Self-healing cannot occur with this disease, so that the person affected is usually always dependent on medical treatment. Facet syndrome is treated in most cases by means of physiotherapy or physiotherapy. In general, it is not possible to predict whether the therapy will be successful.
In many cases, however, those affected can repeat the exercises from this therapy themselves at home, which may accelerate healing. In many cases, patients are also dependent on taking medication, taking care to ensure the correct dosage. If anything is unclear or in doubt, a doctor should always be contacted. Psychological support from friends and family is also very important in facet syndrome so that depression does not occur.
You can do that yourself
Since the articular cartilage is largely nourished and maintained through good blood circulation, there are many opportunities for those affected to help themselves.
Movement promotes blood circulation and thus healing. Facet syndrome can be countered with the help of simple movement exercises on your own initiative. All exercises should be performed with as little body weight as possible. It turns out to be extremely useful to exercise in the water, as your own body weight is minimized to the maximum. When doing the exercises, make sure that they can be performed easily and pain-free. If symptoms arise, the exercise should be interrupted.
The cervical spine is very flexible and delicate and should therefore only be mobilized carefully. In the sitting position, with the back straight, the chin is tilted towards the chest and then gently moved alternately to both sides. The head can also be tilted carefully to the left and right towards the shoulders.
The thoracic spine is relatively immobile and allows rotation and lateral inclination. These can be trained in a targeted manner by spreading both arms and then bringing them together above the head. Furthermore, the hands can be placed one inside the other and the arms can be raised over the head in a wide arc, as with a golf swing.
The lumbar spine can be loosened and strengthened with exercise balls. To do this, the pelvis is tilted into the sitting position, rotated and rolled over the seat humps.