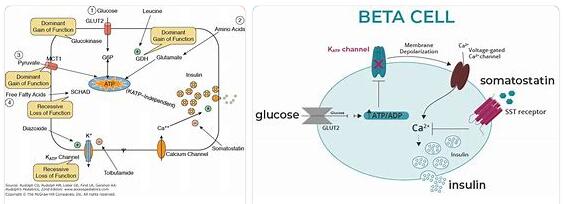
Hyperinsulinism is a condition of increased insulin concentration in the blood, which results in hypoglycemia (low blood sugar). Low blood sugar often causes serious health problems that can lead to coma or even death.
What is hyperinsulinism?
Hyperinsulinism is characterized by constant sweating, tremors and pallor. In congenital hyperinsulinism, these symptoms appear from birth. See AbbreviationFinder for abbreviations related to Hyperinsulinism.
A distinction is made between hyperinsulinism and hyperinsulinemia. While in hyperinsulinemia the insulin concentrations are only temporarily elevated, hyperinsulinism is characterized by permanently elevated insulin levels in the blood. There are several reasons for the increased concentrations in the blood.
The most common is congenital hyperinsulinism, which is genetic and is present from birth. Insulin, a hormone produced by the pancreas, is responsible for regulating blood sugar levels. It ensures the infiltration of glucose into the body cells. The more insulin there is, the more glucose is transported into the cells. The blood sugar level drops more and more and reaches values that are too low.
Therefore, the body can no longer be sufficiently supplied with glucose. The brain is particularly dependent on glucose. If the supply of glucose to the brain is too low, it can no longer adequately perform important functions. In severe cases, coma and death often occur. In milder cases of hyperinsulinism, the body tries to compensate for the hypoglycaemia by eating more.
Causes
Hyperinsulinism can be caused either by permanently increased insulin production in the pancreas or by delayed breakdown of insulin. In most cases, however, more insulin is produced. For example, type II diabetes is caused by reduced insulin resistance.
This means that although there is enough insulin, it is less effective due to the lack of insulin receptors. The pancreas now tries to compensate for the insulin effectiveness by increasing insulin production. However, in this case, the blood sugar level remains elevated or at most reaches normal values.
Hyperinsulinism with hypoglycaemia develops with a special tumor in the pancreas (insulinoma) or with a genetically caused overproduction of insulin. The so-called genetic congenital hyperinsulinism is the most common form of hyperinsulinism. This in turn can be divided into focal and diffuse hyperinsulinism.
In focal congenital hyperinsulinism, there is usually only one affected area in the pancreas. Diffuse hyperinsulinism is characterized by the fact that all islet cells produce more insulin. Insulin production can also be increased by psychological influences or by a slightly reactive pancreas.
Symptoms, Ailments & Signs
Hyperinsulinism is characterized by constant sweating, tremors and pallor. In congenital hyperinsulinism, these symptoms appear from birth. Furthermore, behavioral problems, lethargy, seizures and disturbances of consciousness are observed. Symptoms can be quickly treated with glucose administration.
After that, however, the blood sugar level drops again very sharply. In severe untreated cases, the disease can be fatal or cause severe intellectual development disorders. In the very mild forms of hyperinsulinism, a constant feeling of hunger often leads to increased food intake. As a result, high levels of obesity can occur.
Diagnosis & course of disease
Diagnosis of hyperinsulinism is made through blood tests. Insulin levels, fasting blood sugar in the blood and ketone bodies in the serum are measured. If the insulin level is over 3 U/l in the fasting state and the blood sugar level is low, one can speak of hyperinsulinism.
The concentration of ketone bodies is reduced because insulin inhibits lipolysis and as a result fewer ketone bodies can be formed from the breakdown of fatty acids. Improvement of symptoms by administration of glucose or administration of glucagon also indicates hyperinsulinism. Finally, the pancreatic tissue can be assessed using imaging methods such as sonography.
In addition, sonography is also suitable for excluding a tumor as the cause of hyperinsulinism. When assessing the pancreatic parenchyma, it is important to distinguish between focal and diffuse hyperinsulinism. The distinction is very important for designing the treatment strategy.
Complications
Hyperinsulinism leads to severe hypoglycaemia in the patient. This can lead to various health problems and complications. In many cases, people lose consciousness when they have hypoglycaemia or feel ill and exhausted. The patient’s resilience drops significantly and the heartbeat increases even with light activities.
The affected person also appears pale and can hardly concentrate. Disorders of consciousness occur and the patient suffers from sweating and seizures. The quality of life is significantly reduced by hyperinsulinism. If the disease occurs in children, it can lead to significant developmental disorders, which can usually lead to consequential damage in adulthood.
The feeling of hunger is increased by hyperinsulinism and the patient tends to eat more, which can lead to obesity and overweight. There are no special complications in the treatment of the disease. The main drugs used are those that can eliminate the symptoms relatively quickly. Surgical intervention is only necessary in rare cases. If treated early, the life expectancy of the affected person will not be reduced.
When should you go to the doctor?
People who tend to sweat quickly even with light movements or the performance of everyday tasks should consult a doctor to clarify the symptoms. Nervousness, persistent trembling of the limbs or a pale complexion are indications of discrepancies. A doctor’s visit is necessary as soon as the symptoms persist for several days or weeks and increase in intensity.
Cramps in the body, abnormal behavior or lethargy must be examined by a doctor. If the symptoms occur in a newborn child, the pediatrician must be informed immediately. In the event of disorders of consciousness or loss of consciousness, medical care must take place as quickly as possible to ensure the survival of the person concerned. In severe cases, an ambulance should be called. Until his arrival, first aid measures must be taken and breathing secured. A sudden breakdown, unexpected behavioral problems, or severe mood swings are causes for concern.
In the event of a drop in the usual level of performance, reduced drive and inner restlessness, a visit to the doctor is advisable. General weakness, a strong feeling of hunger and problems with eating should be discussed with a doctor. If there are irregularities in digestion, changes in weight or an increased need for sleep, the observations should be examined by a doctor.
Treatment & Therapy
The treatment of hyperinsulinism depends on its cause. Oral or intravenous glucose substitution is a conservative treatment method. The hormone glucagon can also be substituted. Glucagon is the antagonist of insulin and ensures the breakdown of glucogen stored in the liver into glucose.
At the same time, drug treatment with diazoxide or nifedipine can take place. Diazoxide opens the ATP-sensitive potassium channels. Nifedipine blocks calcium channels. This inhibits insulin secretion. If conservative methods do not improve symptoms, surgical removal of the overactive islet cells can also be considered.
In the case of focal hyperinsulinism, a complete cure is often possible. Only the affected part of the pancreas is removed. In the case of diffuse hyperinsulinism, a complete resection of the islet cells would have to be carried out. In this case, however, type I diabetes develops. Therefore, in this case, attempts are made to achieve the greatest possible success through drug treatment so that no surgery is necessary.
However, it has turned out that there is still an atypical hyperinsulinism that combines both forms of congenital hyperinsulinism. In atypical hyperinsulinism, there are several highly active sites in the pancreas. These can be detected using imaging methods. Here, too, surgical removal of the affected areas can lead to complete healing.
Outlook & Forecast
Hyperinsulinism triggers serious complications if medical care is not sought. The prognosis in these cases is extremely unfavorable. Hypoglycaemia and severe life-threatening consequences occur. The patient may lose consciousness and fall into a coma. This condition is potentially fatal or can cause irreparable damage.
Treatment improves the chances of symptom relief. However, the cause of the hyperinsulinism is decisive. In the case of a tumor disease, the stage and curability of the tumor are decisive for the overall prognosis. If the tumor is discovered early and completely removed, it can be treated with subsequent cancer therapya good prognosis can be given. In most cases, long-term therapy is then initiated, during which there is a significant improvement in the symptoms. If there is no prospect of a cure from cancer therapy, drug treatment is given to alleviate existing symptoms. In these cases, the care of the patient is geared towards alleviating the symptoms of all irregularities in order to alleviate existing suffering.
If the patient suffers from a chronic underlying disease, no cure can be expected. The insulin balance is monitored and regulated. As soon as the prescribed medicines are discontinued, the symptoms recur. If the treatment plan is observed, there is a sustained improvement in the quality of life.
Prevention
Prevention is not possible for most forms of hyperinsulinism. Only the hyperinsulinism caused by type II diabetes mellitus can be prevented by a healthy lifestyle.
Aftercare
In the case of hyperinsulinism, follow-up care proves to be difficult in most cases. In most cases, the measures and options for aftercare are severely limited, so that the person affected is primarily dependent on a quick and, above all, early diagnosis of this disease. In the worst case, if left untreated, it can even lead to the death of the person affected, so that the focus of this disease is on early detection.
The earlier hyperinsulinism is detected, the better the further course of this disease. The disease is often treated by taking medication. It is important to ensure the right dosage with regular intake in order to relieve the symptoms properly and permanently.
If there are any questions or ambiguities, a doctor must always be consulted first. In the event of side effects or interactions, a doctor should also be consulted first. Contact with other patients with hyperinsulinism can be useful, as it is not uncommon for information to be exchanged. It cannot generally be predicted whether the disease will lead to a reduced life expectancy.
You can do that yourself
Hyperinsulinism must always be treated by a doctor. In the worst case, if left untreated, the patient may die.
In the case of diabetes, a healthy diet and a healthy lifestyle can have a very positive effect on the disease. Ideally, the disease can also be completely curbed in this way. As a rule, however, those affected are dependent on medical treatment. Since those affected sweat frequently and profusely due to the disease, light and airy clothing should be worn to avoid sweating.
In the case of behavioral problems or disorders of consciousness, special support for those affected can have a positive effect on the disease. However, the symptoms can be treated relatively easily and quickly by taking medication. Furthermore, patients with hyperinsulinism should take part in regular blood tests to control the blood sugar level. Other examinations of the internal organs are also advisable.
If you lose consciousness from hypoglycaemia, you should call an ambulance. Until the arrival of the emergency doctor, the person concerned must be placed in a stable lateral position. Breathing should also be regular and calm.