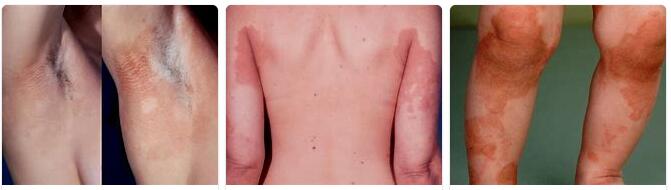
The Erythrokeratoderma is a disease of the skin, which belongs to the group of keratoderma. It is a disease that causes the outermost layer of skin to thicken and reddened skin. This thickening of the skin is also known as cornification or hyperkeratosis and the reddening of the skin is erythroderma.
What is erythrokeratoderma?
According to percomputer.com, Erythrokeratoderma belongs to the subgroup of hereditary palmoplantar keratosis. This skin condition, in turn, belongs to the keratoderma family. Erythrokeratoderma is divided into four other diseases:
These are Erythrokeratodermia progressivia symmetrica, Erythrokeratodermia variabilis, Erythrokeratodermia papillaris et reticularis and Erythrokeratodermia en cocardes Degos.
In erythrokeratoderma, keratinization of the skin on the hands and feet occurs together with reddening of the skin due to inflammation. This reddening of the skin is also known as erythroderma. Erythroderma can also occur independently of erythrokeratoderma or as a subsequent disease in other dermatological diseases.
The skin is the human protective barrier against external influences from the environment such as UV rays. The skin consists of several layers, the outer layer being formed by the epidermis. This in turn is formed by further layers. The innermost layer is the basal layer, also called the stratum basale.
Further outwards follow the prickly layer or stratum spinosum, the granular layer or stratum granulosum, the glossy layer or stratum lucidum and finally the outermost layer, which is the horny layer or stratum corneum. The epidermis consists of a certain type of cell, the keratinocytes. They produce keratin and keratinize when they migrate from the basal layer to the horny layer.
These cells die in the process. The horny layer consists of dead and keratinized keratinocytes, which are then referred to as horn cells or corneocytes. A disruption in this process can lead to increased keratinization of the skin. There is an increased production of corneocytes, which accumulate in the cornea and lead to thickening of this skin layer.
This process is known as hyperkeratosis. With erythrokeratoderma, there is also erythroderma, the reddening of the skin due to inflammation.
Causes
Like most keratoderma diseases, erythrokeratoderma is hereditary. However, it can also appear as a side effect of other diseases. Erythrokeratodermia can develop if the person concerned suffers from other diseases such as ataxia, congenital non-bullous ichthyosiform erythroderma, hypotrichosis-deafness syndrome or bullous congenital ichthyosiform erythroderma.
There is an increased formation of corneocytes, which are deposited in the cornea, or the body is no longer able to renew the cornea naturally. Erythroderma is divided into primary and secondary erythroderma. Primary erythroderma occurs when the person concerned previously had another disease. Then it is divided into acute or chronic erythroderma.
Acute erythroderma requires rapid treatment, as otherwise a life-threatening situation can arise. Chronic erythroderma is less aggressive than the acute form and is inherited as is the case with erythrokeratoderma. Secondary erythroderma is the form that is developed as a result of previous dermatological diseases. This is the most common type of erythroderma.
Symptoms, ailments & signs
Erythrokeratoderma is characterized by two major underlying diseases. There is a hyperkeratosis, the keratinization of the skin on the hands and feet. This occurs through the formation of dandruff. In addition, there is erythroderma. Erythroderma is an inflammation of the skin together with a dilation of the blood vessels.
This leads to the visible reddening of the skin in erythrokeratoderma. Depending on the severity of the erythroderma, there can be severe losses of fluids and nutrients such as salts. The widened vessels also lead to an increased loss of body heat to the environment. The result is increased sensitivity at cold temperatures.
Diagnosis & course
The diagnosis of erythrokeratoderma is made by a specialist in dermatology. The keratinization of the hands and feet as well as the reddening of the skin due to inflammation and vasodilatation are clearly visible. If the erythrokeratoderma is not treated, the cornifications can spread.
The keratinization of the skin can also continuously increase, so that the mobility of the hands and feet can be impaired. If erythroderma is also not treated, there can be a severe loss of fluids and trace elements, which can cause extensive damage to the body. It can also lead to a life-threatening situation for the person concerned.
Complications
With erythrokeratoderma, the patient suffers primarily from cosmetic complications, as it is a severe thickening of the skin with redness. These symptoms can lead to decreased self-esteem and also to inferiority complexes. Pronounced erythrokeratoderma also leads to a loss of nutrients and fluids.
The affected person can also lose body heat and suffer from cold extremities as a result. The temperature sensitivity also increases, which can lead to unpleasant feelings and pain on the skin, especially in cold temperatures. Without treatment, very high losses of important nutrients and trace elements occur.
These losses can cause harm to the body in the long run and have a negative impact on health. The exact complications depend on the amount of loss. Usually, erythrokeratoderma can be treated relatively well with medication to limit symptoms.
There are no further complications. If treated early, life expectancy will not be reduced. However, if the body continues to lose fluids and nutrients, the cardiovascular system can be damaged.
When should you go to the doctor?
A doctor’s visit is necessary if there are unusual changes in the complexion of the skin. A thickening of the upper layer of the skin should be examined medically to determine the cause. Consult a doctor if sensory disturbances occur or if you feel numb. The formation of scales on the skin indicates dehydration. This should be treated medically, as it can lead to feelings of tension and cracks. In the case of open wounds, germs can enter the organism and trigger further diseases.
In severe cases there is a risk of blood poisoning. A doctor should be consulted as soon as there are further symptoms or pain in the affected areas. Reddening of the skin or the loss of body fluids through the skin must be examined by a doctor. If the temperature sensitivity increases or if the hands and feet cool down unusually quickly, these symptoms should be presented to a doctor.
If the gait changes due to the symptoms or if there is a loss of strength, a doctor’s visit is necessary. If you feel generally unwell, or if the affected region has spread, you should also consult a doctor. If the person concerned suffers emotionally or mentally from the visual flaw, it is advisable to talk to a doctor about various options for relief.
Treatment & Therapy
Hyperkeratosis can be treated by a dermatologist with the help of keratolytics. Keratolytics include benzoyl peroxide, azelaic acid, alpha-hydroxy acids, urea and retinoids. They soften the cornea. It can then be removed with various aids such as a pumice stone or a corneal rasp.
Erythroderma is treated with glucocorticoids. This treatment is essential as it can cause dehydration and excessive stress on the cardiovascular system. In addition, the patient is given sufficient fluids to counteract erythroderma.
Outlook & forecast
The hereditary disease can only be treated symptomatically by doctors. Since doctors are not allowed to change human genetics for legal reasons, a complete cure is not possible according to the current status. However, the symptoms can be significantly alleviated by using medical care. Therapy takes place through the administration of medicines. The active ingredients soften the cornea so that the unwanted tissue can be removed manually and independently.
Without treatment, there is a long-term loss of nutrients and trace elements through the skin. In this way vital elements are withdrawn from the organism and a deficiency symptom occurs. The prognosis worsens significantly under these conditions. There is a risk of cardiovascular stress and dehydration. This means that there is a potentially life-threatening condition for the person affected.
With medical care, this development can almost be ruled out. Due to the removal of the cornea and an adequate supply of the skin, the loss of nutrients is curbed. Long-term consequences are not to be expected under these conditions. The care of the skin is carried out in a lifelong therapy. As soon as this is interrupted or broken off, the cornea develops within a short time. This leads to a relapse of the symptoms and a worsening of the prognosis.
Prevention
Erythrokeratoderma is a hereditary disease. Therefore there are no preventive measures. As soon as the disease appears, it must be treated in order to avoid consequential damage.
Aftercare
In most cases of erythrokeratoderma, the patient has only very limited options for follow-up care. The person concerned is therefore dependent on treatment by a doctor, whereby a quick and above all early diagnosis of the disease is primarily important in order to prevent further complications. The earlier the erythrokeratoderma is detected, the better the further course of this disease is, as a rule.
With erythrokeratoderma, patients are dependent on taking drugs that can permanently alleviate the symptoms. It is important to ensure that it is taken correctly, and the person concerned should always discuss interactions and side effects with a doctor. In case of doubt, a doctor should always be consulted. Furthermore, the person concerned should always take care of his body and not stress it unnecessarily.
Consuming plenty of fluids can also have a positive effect on the course of erythrokeratoderma and prevent further symptoms. In most cases, this disease will not reduce the patient’s life expectancy. Contact with other people affected by the disease can also prove to be useful, as this often leads to an exchange of information.
You can do that yourself
The hereditary disease offers the patient little scope for self-help. In everyday life, the self-help measures are to be understood as support for the conventional medical guidelines, which are intended to improve well-being.
Erythrokeratoderma patients can use coordinated skin care products to improve their skin quality and thus alleviate some symptoms. Creams and ointments that contain a lot of liquid are particularly recommended. In addition, there are special fluids that can be used for rapid callus formation. If possible, the care products should be applied to the desired skin areas several times a day.
At the same time, wearing synthetic clothing should be avoided. These dry out the skin and lead to an increase in symptoms. When spending time in swimming pools or public bathing establishments, the feet should be cared for particularly intensively, as the chlorine contained in the water also allows the skin to dry out.
With various rasps or stones to remove calluses, the patient can independently remove the dead skin layers. Medical foot baths also support the skin and prevent cracking. These can be carried out independently as required. The entire body must be kept from dehydration. To do this, the recommended amount of fluid should be consumed daily.